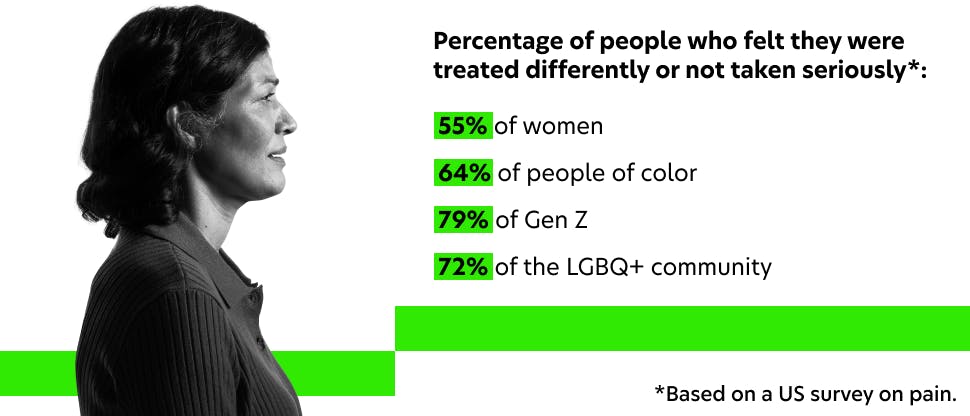Their pain is never just one word
Start the conversation
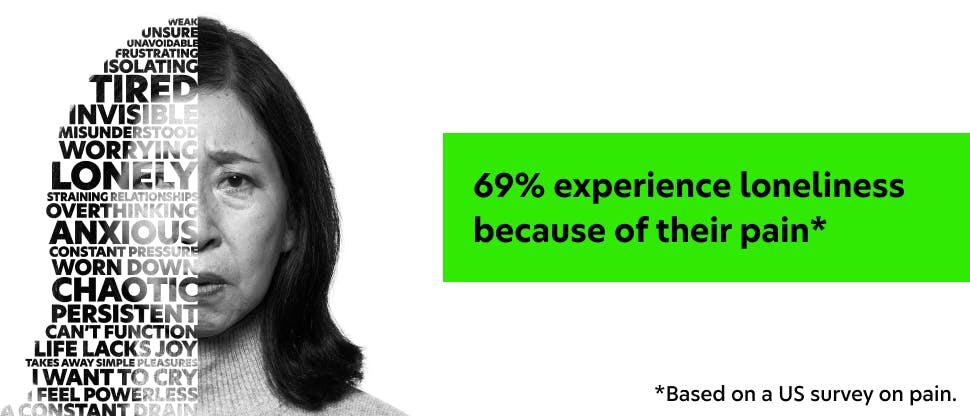
No one knows the impact of pain better than those afflicted by it. For some, it can be hard to express—because pain is never just one word. Each person has their own unique challenges and journey with pain, making pinpointing the root cause feel like an uphill battle. So how can you explore a patient’s pain experience to provide the best treatment? It starts by asking the right questions.
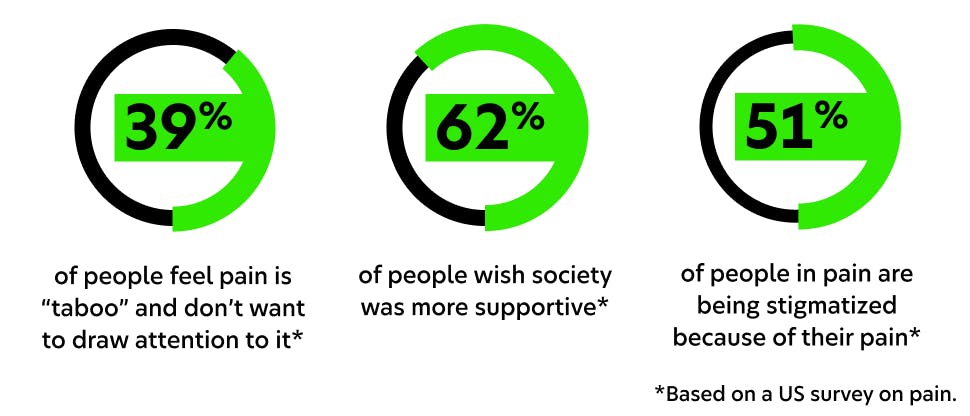
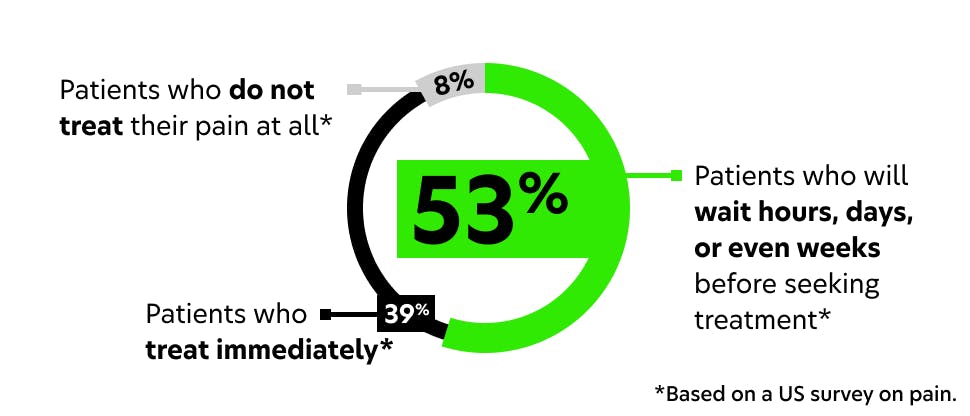
Our latest Haleon Pain Index reveals insights from both healthcare professionals (HCPs) and patients about the impact of pain and how to create positive change.
The Haleon Pain Index (previously known as the Global Pain Index) 5th edition conducted 18,000+ interviews with consumers in 18 countries and 600+ HCPs in 4 countries including the US. It uncovers the perceived impact of pain in patients’ everyday lives—on their health, emotions, motivations, and behaviors—to focus on the human experience. The Haleon Pain Index is anchored in Haleon’s commitment to deliver better everyday health with humanity by breaking down the barriers between HCPs and patients to improve clinical outcomes.
See the pivotal insights from the Haleon Pain Index US fact sheet now.
Better conversations for better clinical outcomes in pain management

A helping hand from Haleon
At Haleon, we believe in making sure that every patient gets exactly what they need to manage their unique pain experience. The #ListenToPain campaign aims to equip HCPs with the knowledge and tools to better understand their patients’ pain. Using information from the Haleon Pain Index, we’ve established five different patient profiles, describing their relationship with and the handling of their pain. Based on a deep understanding of the human pain experience, these five profiles can help you maximize those precious minutes with patients and individualize your approach.
We’re committed to providing HCPs with new tools and techniques and sharing the latest advances in pain management—innovation that will allow you to better #ListenToPain.
Discover more pain management resources below

#ListenToPain Tools & Resources
Access resources designed to help your patients navigate pain management.

#ListenToPain Patient Profiles
Discover different patient profiles to understand the person behind the pain.

The Advil Pain Equity Project
Learn more about how we are helping to address pain bias through research, education, and collaboration.